 
That said, many of our patients simply “don’t read the textbook” - and recognition of hyperkalemia becomes much more challenging when T wave peaking isn’t obvious (ie, when T waves aren’t so pointed with such a narrow base - or, when other abnormalities such as RBBB are present). Smith’s ECG Blog has trouble recognizing hyperkalemia when all of the typical findings are present. NOTE - I would bet that No One who regularly follows Dr.Meyers appropriately suggests that empiric Calcium would be a reasonable option in this circumstance, even before knowing the serum K+ level. Meyers - the combination of QRS widening + bradycardia + lack of sinus P waves should immediately suggest the possibility of Hyperkalemia - especially since T waves in no less than 8/12 leads (ie, in leads I,II,aVL,aVF and in V3-thru-V6) in the initial ECG look more-peaked -than-they-normally-should-be. Superb interpretation of the presenting ECG in this case by Dr. Apparently the patient was mentating and had a normal blood pressure with this, and did not require pacing at that moment. Otherwise, this would be complete heart block with junctional escape. If the possible atrial waves are real, it could be sinus bradycardia with 2:1 AV block. There are possible atrial waves but it is not definitive with this low quality ECG. The slight ST elevation is diagnostic of posterior STEMI, which in posterior leads only requires 0.5 mm in just one lead to meet "criteria." How do we know? We can tell this because of the very low QRS amplitude and the Q-waves. These are almost certainly posterior leads, though they were not labelled as such (V4-V6 are really V7-V9 on the posterior thorax). This just goes to show that there are always false positives and false negatives. V4 and V5 especially have the appearance of hyperK. Smith comment: When Pendell texted this to me, I thought it was both hyperkalemia and inferior posterior OMI. Cardiology was recalled to bedside to reevaluate. The initial troponin T returned highly elevated at 4.04 ng/mL. We have shown several cases on this blog that appear to have both OMI and severe hyperkalemia.Īdditionally, both 1) no spontaneous sinus activity (sinus arrest or extreme sinus brady) and 2) no retrograde activity, which implies AV block as wellĬardiology was summoned immediately to bedside but they thought that this ECG "isn't a STEMI" and refused to take the patient to the lab. Along with bradycardia and conduction block, this would be alarming for potential hyperkalemia, which of course can also cause OMI mimics. Interestingly, many of the T waves have a slightly peaked appearance. The inferior leads show Q waves with STE in lead III, and there is some slight reciprocal STD in I and aVL. This STD is excessively discordant in V2, and concordant in V3. Alternatively, it could be a posterior fascicular escape. There is STD in V2-V5 that is maximal in V2 and V3. Interpretation: There is an absence of sinus activity, including an absence of retrograde P waves. The rhythm is probably a junctional escape at a rate of approximately 45, with RBBB and likely also LAFB (given the leftward axis despite RBBB). Either LCX or RCA, or perhaps an Obtuse Marginal that supplies those regions." I'd also give a little calcium because it's slow, wide, and a couple leads have almost pointy Ts. 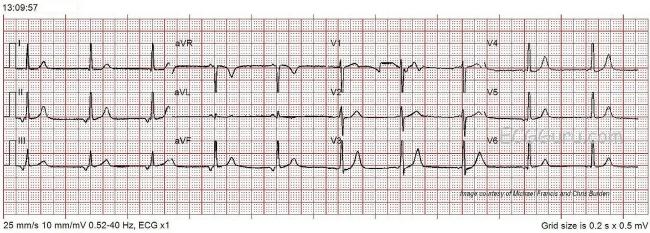
"It's posterolateral (and probably also inferior) OMI until proven otherwise. 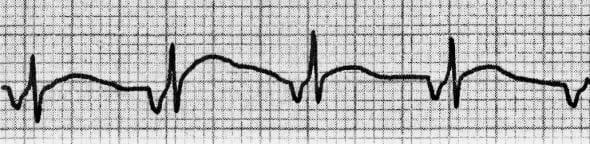
This case was sent to me with only the details above, and my response was:
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
